MASS MONSTER OR FAT BLOKE? THE PERILS OF BODY MASS INDEX FOR FIT PEOPLE
Mass Monster Or Fat Bloke? The Perils Of Body Mass Index For Fit People
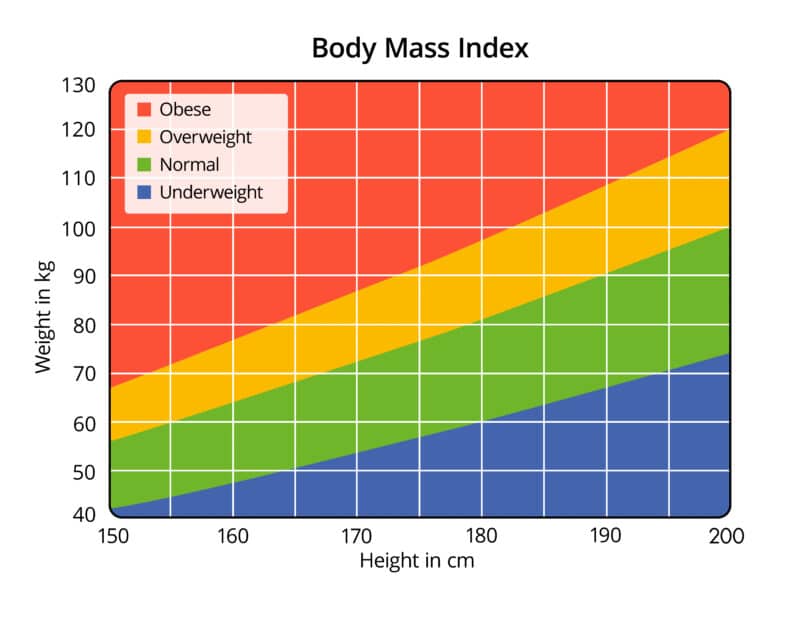
Body Mass Index
(Click on the Reference Numbers in Blue for More Info)
If you engage in some form of resistance training and carry more muscle than the average person, there is a good chance that you may have been told by a health care professional that you are overweight or even obese, despite the fact that you may be relatively lean. This may have left you feeling confused or perhaps annoyed to find out that despite all of your hard work in the gym and strict dieting, according to the medical profession you are considered to be at a greater risk of developing a range of health problems, such as diabetes, cardiovascular disease and certain cancers, because of your ‘weight’.
Don’t worry; you are not alone. This is a common problem for bodybuilders, strength athletes and pretty much anyone who engages in heavy resistance training. The problem lies in the way in which your level of health risk has been calculated, which typically involves the use of a formula referred to as Body Mass Index. In this article, we are going to explain what BMI is, why it can be problematic for those carrying greater than average levels of muscle, its pros and cons, how race can affect BMI, how BMI should be used, and how you can find out if your ‘weight’ is a potential threat to your health.
The traditional approach to bodyweight and health risk
The traditional approach to determining the health risks associated with body weight was actuarial- based height-weight tables or charts, which you may have seen on the wall of your doctor’s surgery. These were used to assess the ‘overweightness’ of a person based on height and weight. The problem with such tables is that they do not provide data on the composition of an individual (1); that is, the relative proportions of fat and lean mass in the body expressed as a percentage of body weight. Consequently, a person may weigh much more than is recommended for their height because they carry a considerable amount of muscle and may have low body fat, but still be considered at risk of the health conditions associated with obesity. More recently Body Mass Index has typically been used to assess an individual’s weight related health risks.
What is Body Mass Index?

Body mass index, also known as the Quetelet index, is a mathematical formula used to determine a person’s weight relative to their height. It is calculated by dividing body weight in kilograms by height in metres squared (w/ht2) (1).
For example, if you weigh 70kg and are 1.75m tall you will have a BMI of 22.9.
BMI = 70 kg / (1.75 m2) = 70 / 3.06 = 22.9
It is used to classify people as underweight, overweight and/or obese.
As a quick guide you are considered to be:
- Underweight if you BMI is less than 18.5
- Normal weight if your BMI is 18.5-24.9
- Overweight if your BMI is 25.0-29.9
- Obese if your BMI is 30 or greater (2)
To save you doing the maths, just click on the link below to the NHS BMI calculator to find your own BMI:
BMI calculator | Check your BMI – NHS | Please fill in your details (www.nhs.uk)
How accurate is BMI?

You may be thinking how is BMI any more accurate than the standard weight and height charts if it’s just based on weight and height? It is considered to have a somewhat higher association with body fat because of the mathematical calculation that divides body mass by height squared (1). It has been suggested that BMI can be used to predict percentage of body fat. However, as the standard error of estimating %BF from BMI is plus or minus 5%, it is recommended that other more accurate methods be used to assess body composition (3). That said, with exception of individuals with large amounts of muscle mass, it is well established that, those with a BMI of more than 30 have excess body fat (3).
How does race affect BMI?
Until recently it was assumed that the relationship between BMI and the level of fat an individual has is the same for all races, but this is not the case (4). For example, Asians have a higher percentage of body fat than Caucasian people of the same age, sex and BMI (5). Black, Asian and other minority ethnic groups have a higher risk of developing certain long-term conditions related to increased levels of body fat, such as type 2 diabetes. Therefore, the NHS suggests that adults in these groups with a BMI of:
23 or more are at increased risk
27.5 or more are at high risk (6)
Consequently, they will need to maintain a lower BMI than their white peers to be healthy.
Advantages and limitations of BMI
The main advantages of BMI are that it is inexpensive, simple and quick. It is useful as a population-level measure of being overweight and obese as it is the same for both sexes and for adults of all ages (7).
On the other hand:
- It tends to overestimate the fatness of people that are very muscular, such as body builders.
- Conversely, it can underestimate fatness in people who have lost muscle mass, such as the elderly (3), whomay fall into the ‘healthy weight’ range even though they may be carrying excess fat.
- It does not adequately reflect changes in fat and muscle mass that occur as a result of weight loss nor does it indicate where an individual’s fat is deposited (1).
- People who are less than five feet tall may have a high BMI that does not reflect their true body fat levels. This also applies to people suffering from excessive accumulation of fluid in the tissues of the body (5).
Waist to height
This may leave you thinking how can I find out if my weight is a potential health issue if BMI is not appropriate for me? Research has shown that the ratio between our height and waist is a better predictor of health risk than BMI (8). This is because where we store fat on our body appears to have a greater influence on the health risks associated with obesity rather than our total amount of body fat (3).
Individuals who are apple shaped (android obesity), in which fat is mainly deposited on their trunk (abdominal fat) have a greater risk of suffering from obesity related conditions, such as type 2 diabetes, and cardiovascular, etc, compared to individuals with gynoid obesity (pear shape), in which the fat is deposited on the hips and thighs (1).
Ideally, we should aim to keep our waist measurement less than half that of our height (8). For example, a man 6ft (182.88 cm) tall should aim to keep his waist less than 36 inches (91.4 cm), while a 5ft 4in (162.56 cm) woman should keep hers under 32 inches (81.28 cm).
How to take your waist measurement
- Stand with your feet together and your abdomen relaxed
- Find the bottom of your ribs and the top of your hips
- Breathe out normally
- Wrap a tape measure around your waist, midway between these points, without compressing the fat
- Ensure that the tape measure is horizontal
- Record the measurement to the nearest centimetre (9)
Note: Waist circumference can be less accurate in certain circumstances including pregnancy, when an individual is suffering from a condition that cause distension of the abdomen, for certain ethnic groups, and for children and young people.
Assessing body composition
Although BMI and waist measurements can be used to assess health risk, they are not measures of body composition, as they do not provide indication of our percentage of body fat. If you wish to know how much body fat you have, there are now a wide variety of techniques available to assess body composition. These range in complexity, accuracy and expense from simple circumference measurements made using inexpensive tape measures and skinfold callipers to DEXA scans which employ expensive high-tech equipment to produce radiographic images of the body.
Time for some controversy

Although this seems contrary to everything we have said so far, there is evidence to suggest that in certain circumstances a higher BMI than would typically be recommended may be healthy. For example, patients with congestive heart failure have been shown to have an improved survival rate when their BMI is 30 or greater (3). This phenomenon is known as the ‘obesity paradox’.
A study found that the BMI linked to the lowest risk of dying from any cause has increased over the last few decades from 23.7 in the 1970s, 24.6 in the 1990s, and to 27 in the 2003-13 period (4).
The main argument against the use of BMI (Body Mass Index) for those carrying a large amount of muscle mass is that it is an excess of bodyfat that is harmful to health not being heavy per se, and, as we have seen, there is some evidence to suggest that being a bit heavier may be healthier. However, in recent years concerns have been raised in the bodybuilding community over the potential health consequences of carrying extremely high levels of muscle mass as exhibited by some modern bodybuilders, despite their low levels of body fat.
It seems that there is some scientific evidence to support this concern. A study by Ortega et al., (10) found that having a very high BMI was a significantly stronger predictor than a very high percentage of body fat on cardiovascular mortality. The authors concluded that despite BMI being a poor index of body composition, because it does not discriminate between fat mass and fat free mass (i.e. all tissues that are not fat including muscle, bone, organs), it is perhaps a very good index of future health/disease, and particularly for cardiovascular disease. The explanation for this finding seems to be related to the fact that a very high level of fat free mass was also positively associated with a higher risk of CVD death.
To confuse things further, the results of a study by Tyrovolas and colleagues (11), which investigated the effects of skeletal muscle mass in relation to cardiovascular disease incidence among middle aged and older adults, found that participants with greatest amount of skeletal muscle had a reduced risk of cardiovascular disease in comparison with those with the lowest levels.
Body Mass Index Conclusion
Understanding the limitations of BMI will allow us to use it with good judgement and so enhance its accuracy. As we have seen, there would be little point in using BMI with a person who has a large muscle mass nor someone who has lost a significant amount muscle due to age or disease, but for most other people it can provide an indication of an individual’s risk of obesity related disease when used appropriately. It is important to note that although there is some evidence to suggest that a BMI slightly higher than currently recommended may be healthy, the current guidelines should be adhered to until there is more comprehensive evidence to support raising the BMI threshold. Likewise, although there is some evidence that very high levels of muscle can pose a potential threat to health, so too can low levels. The bottom line is that having too much body fat can be prejudicial to good health and at very high levels, muscle can also be problematic. Like most things in life, health and fitness, it would seem to be a question of balance.
To read our Time 4 Fat Loss Series – Part 1 – Why Do We Get Fatter?, please click the link below.
